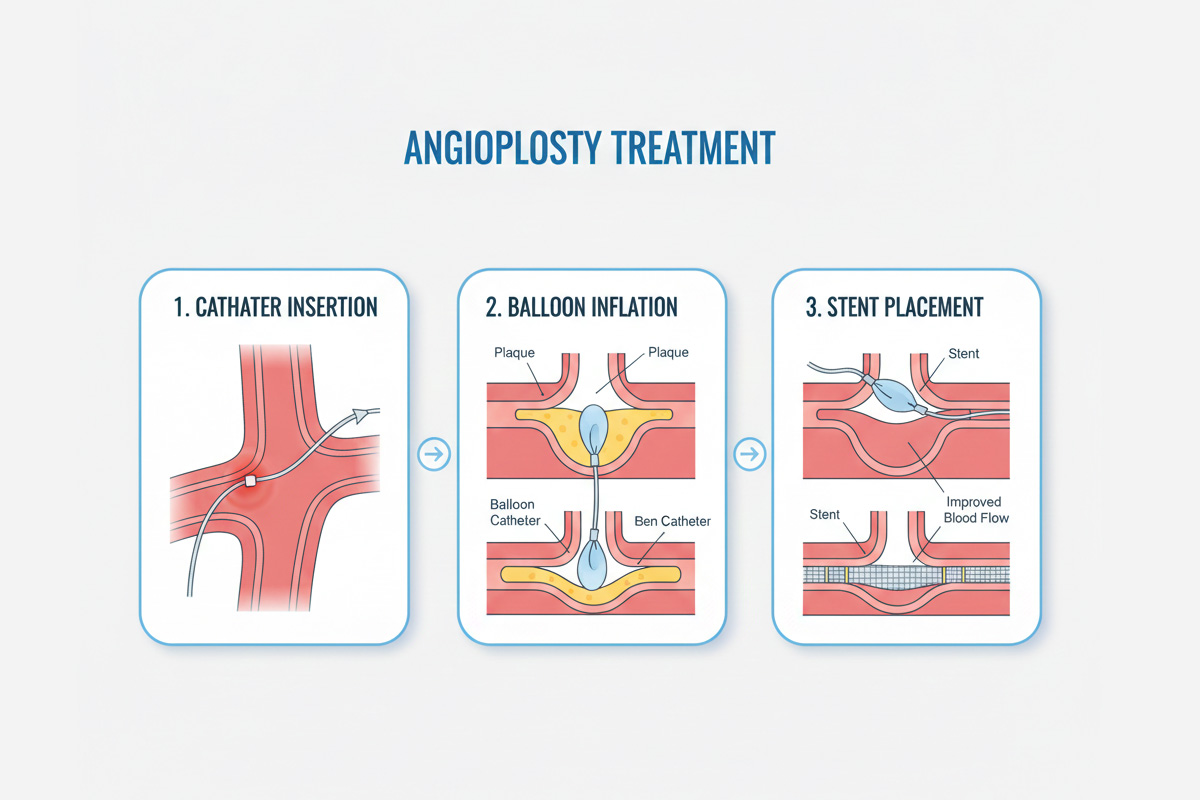
WHAT IS ANGIOPLASTY OR BALLOON ANGIOPLASTY?
Angioplasty, also called balloon angioplasty, and vascular stenting are minimally invasive procedures performed to improve blood flow in the body’s arteries. This procedure is similar to Angiography up to the introduction of the catheter.
In the angioplasty procedure, the catheter is balloon-tipped—and this thin, plastic tube—is inserted to the site of a narrow or blocked artery and then the balloon is inflated to open the vessel. The balloon is then deflated and removed from the artery. Vascular stenting, which is often performed at the same time as an angioplasty, involves the placement of a small wire mesh tube called a stent in the newly opened artery. This may be necessary after some angioplasty procedures if the artery is very narrowed or completely blocked.
WHAT IS A STENT?
The stent is wire mesh tube -a permanent device- that is left in the artery and may be needed to help the artery heal in an open position after the angioplasty. The inside of the mesh being hollow allows free flow of blood while supporting the blood vessel.
Stents are categorized according to the benefits provided by them after being placed inside the artery. A normal stent is the wire mesh tube only while a medicated stent has a coating of specific medicine to prevent clotting and blockage subsequently-up to its life period.
WHAT ARE THE USES OF ANGIOPLASTY?
Narrowing or blockage in the arteries is most often caused by atherosclerosis also called hardening of the arteries. Although it is commonly thought of as a heart disease, atherosclerosis can affect arteries anywhere in the body, including the legs and the brain. It is a gradual process in which cholesterol and other fatty deposits—called plaques—build up on the artery walls. These plaques act as barriers that limit blood flow through the arteries to tissues and organs. Other barriers to adequate blood flow include clots or plaques that break away from the blood vessel wall and become lodged in an artery.
When a blood clot, plaque or scar tissue cause an artery to become narrow or completely blocked, blood circulation is limited and the organs and tissues supplied by that artery do not receive enough oxygen.
Angioplasty and vascular stenting are commonly used to treat conditions that result when arteries throughout the body become narrowed or blocked, including:
- Peripheral artery disease (PAD) (narrowing of the arteries in the legs or arms).
- Renal Vascular Hypertension (high blood pressure caused by narrowing of the kidney arteries).
- Hemodilysis access maintenance.
- Carotid Artery disease (narrowing of the neck arteries supplying blood to the brain).
- Coronary artery disease (narrowing of the heart arteries).
Peripheral vascular disease (PVD), also called peripheral artery disease (PAD), is a condition in which there is insufficient blood flow through the arteries to the arms or legs, causing pain ➜, cramping or heaviness in the muscles (called intermittent claudication). Causes of PVD and PAD include atherosclerosis, scar tissue and blood clots. In patients with PVC or PAD, angioplasty may be used to open up a blocked artery in the pelvis, leg or arm. A common site is the iliac arteries of the pelvis.
Renal vascular hypertension is a condition in which one or both of the arteries that supply blood to the kidneys narrow significantly due to atherosclerosis. This reduced blood flow through the renal artery causes the kidney to release increased amounts of the hormone renin, which is responsible for regulating blood pressure. The increase in renin begins a series of chemical events in the body that result in hypertension, also called high blood pressure. Angioplasty and stenting are used to improve blood flow and reduce blood pressure.
Hemodialysis access maintenance: Patients with kidney failure must have regular hemodialysis treatments to prevent waste products from building up in the blood. Some of these patients have a graft (a synthetic material) constructed between an artery and vein in the arm so that blood can easily be withdrawn and replaced during dialysis. On average, these grafts stay open for about one year. Repeated angioplasty can help a graft stay open for as long as five years. Many patients have an arteriovenous fistula, a connection made between the artery and vein that can be used for dialysis. In some cases angioplasty may be used to help these connections work better.
Carotid artery disease is a condition in which there is decreased blood flow in one or both of the carotid arteries, large arteries in the neck that are the major routes of blood and oxygen to the brain. Not enough blood flow to the brain can lead to astroke. A stroke can also result when a piece of plaque breaks off or a blood clot forms, blocking a narrowed or smaller artery of the brain.
Coronary artery disease (CAD), also called coronary heart disease (CHD), results when the coronary arteries—the blood vessels that carry blood and oxygen to the heart muscle—become clogged with plaque due to atherosclerosis.
WHAT AM I REQUIRED TO DO BEFORE ANGIOPLASTY?
Before the procedure several tests are performed – these will be:
- X-ray
- ECG
- Blood test
- Discontinuation of some medicines if required.
- Assessment of your allergy to contrast material or any other medicine
- Discussion of the case with a Cardiac Surgeon to undertake emergency surgery in case of any eventuality during the procedure.
You will be asked not to eat or drink anything after midnight on the night before your procedure. In most cases, you should take any medications that you usually take, especially blood pressure medications. These can be taken with some water in the morning before your procedure. If you are on any blood thinning medication such as Coumadin, you should check with your doctor about if and when you should stop the medication. It is a good idea to check with the Doctor about which medications you should take. You should plan for stay at the hospital – overnight or for a period of 3-4 days and have someone drive you home when you are ready to leave.
WHAT IS THE PROCEDURE FOR ANGIOPLASTY?
To perform an angioplasty, an interventional cardiologist or vascular surgeon makes a small nick in the skin and inserts a balloon-tipped catheter.The catheter is threaded through the artery until it reaches the site of the blockage, where the balloon is inflated, then deflated and removed. Expanding the balloon helps to restore blood flow by stretching the arterial wall, which increases the inner diameter of the artery.
Many angioplasty procedures also include the placement of a stent, a small, flexible tube made of plastic or wire mesh to support the damaged artery walls. Stents are typically placed over a balloon-tipped catheter, which is expanded, pushing the stent in place against the artery wall. When the balloon is deflated and removed, the stent remains permanently in place, acting like a scaffold for the artery.
Drug-coated (also called drug-eluting) stents have recently been approved for clinical use in the coronary (heart) arteries by the U.S. Food and Drug Administration (FDA). These stents are coated with a medication that is slowly released to help keep the blood vessel from re-narrowing, a condition called restenosis. Restenosis, or re-narrowing of the artery can occur with stents, which is why they are not used in all situations. If the artery has opened well with the angioplasty, the stent may not be necessary.
DO I EXPERIENCE ANY PAIN OR DISCOMFORT DURING ANGIOPLASTY?
An intravenous (IV) line will be inserted into your arm so that you can be given a mild sedative and other medications as necessary during the procedure. Although this sedative will make you feel relaxed and drowsy, you will probably remain awake during the procedure. Devices to monitor your heart rate and blood pressure will be attached to your body.
Next—depending on which artery your physician is using for the procedure—your groin area, wrist or arm will be cleaned, shaved and numbed with a local anesthetic. A short tube called a sheath is commonly inserted into the artery. Next, the physician will insert a catheter (a long, flexible tube) through the sheath and advance it to the site of the blockage. An x-ray camera connected to a video monitor will help the physician guide the catheter. You may experience a dull pressure where the physician is working with the catheters, but no pain.
Once the catheter is in place, contrast material will be injected into the artery and an angiogram will be taken of the blocked artery to help identify the site of the blockage. With x-ray guidance, a guide wire will then be advanced to the site, followed by the balloon-tipped catheter. Once it reaches the blockage, the balloon will be inflated for several seconds. The same site may be repeatedly treated or the balloon may be moved to other sites. It is common for patients to feel some mild discomfort when the balloon is inflated because the artery is being stretched. Your discomfort should disappear as the balloon is deflated.
Additional x-ray pictures will be taken to determine how much the blood flow has improved. When your physician is satisfied that the artery has been opened enough, the balloon catheter, guide wire and guiding catheter will be removed. The entire procedure usually lasts 30 minutes to two hours. The length of the procedure varies depending on the time spent evaluating the vascular system prior to any therapy, as well as the complexity of the treatment.
When the procedure is completed, you will be moved to a recovery room or your hospital room. You may feel groggy from the sedative. The catheter insertion site may be bruised and sore. If the sheath was inserted into your arm or wrist, it will be removed and the site will be bandaged. If the catheter was inserted into your groin, you may need to lie in bed with your legs straight for several hours. In some cases, your physician may use a device that seals the small hole in the artery; this may allow you to move around more quickly.
For several hours, your catheter site will be checked for bleeding or swelling and your blood pressure and heart rate will be monitored. Your physician may prescribe medication to relax your arteries, to protect against spasm of the arteries and to prevent blood clots. If a contrast material was used during the procedure, you will urinate often to rid your body of this material. You may be asked to drink extra fluids.
After you return home, you should rest and drink plenty of fluids. You should avoid lifting heavy objects, strenuous exercise and smoking (smoking you should avoid permanently since this is a major cause of atherosclerosis). If bleeding begins where the catheter was inserted, you should lie down, apply pressure to the site and call your physician. Any change in color in your leg, pain or a warm feeling in the area where the catheter was inserted should be reported to your physician.
You should be able to return to your normal routine by the following week.
After an angioplasty or stent placement procedure you may be instructed to take one or more medications (such as aspirin, Plavix, Lovenox or Coumadin) for a period of time. These medications can prevent blood clots from forming at the site of arterial treatment during healing. The effect of Coumadin will be monitored with frequent blood tests.Magnetic resonance imaging (MRI) can probably be done immediately following stent placement, but make sure that you notify the MRI department that you have recently had a stent. Metal detectors will not affect a stent.
Commonly, patients stay overnight and return home the day after the procedure. You will typically be able to walk within six hours following the procedure. You may be required to stay for up to 3 -4 days also, if required. You should be prepared for this.
WHAT ARE THE ADVANTAGES OF ANGIOPLASTY?
- Compared to surgical interventions such as bypass surgery, balloon angioplasty and stent placement are much less invasive and relatively low-risk, low-cost procedures.
- These procedures are performed using local anesthesia; no general anesthetic is required.
- No surgical incision is needed—only a small nick in the skin that does not have to be stitched closed.
- You will be able to return to your normal activities shortly after the procedure.
ARE THERE SOME RISKS OF ANGIOPLASTY?
- Major complications following angioplasty are uncommon. However, inserting the catheter can lead to injury of the artery. The balloon also poses a risk of blood clots or tearing the artery.
- When angioplasty is performed alone, blockages can recur, although most of these arteries can be opened again successfully. This can also occur when a stent is placed in the artery at the time of the angioplasty.
- Heavy bleeding from the catheter insertion site may require special medication or a blood transfusion.
- There is a risk of stroke when angioplasty and/or stenting are performed on the carotid artery.
- A relatively rare complication associated with balloon angioplasty is abrupt vessel closure. This blockage in the area treated by the balloon angioplasty typically occurs within 24 hours of the procedure. If it happens, treatment with medication into the artery to dissolve clots followed by angioplasty or stenting may be appropriate. In some cases, emergency bypass surgery may be needed.
- Other rare complications include heart attack and sudden cardiac death.
WHAT IS RESTENOSIS AND WHAT ARE THE LIMITATIONS OF ANGIOPLASTY?
Restenosis is the deposit of arterial plague after angioplasty. Angioplasty with vascular stenting is just one way to treat narrowed or blocked arteries. Medications and exercise are often the first step in treating atherosclerosis.
Regardless of which artery is blocked, angioplasty does not reverse or cure the underlying disease of arteriosclerosis. It is important for patients to make lifestyle changes, including eating a healthy diet that is low in saturated fat, getting adequate exercise and not smoking. Individuals with diabetes, high blood pressure and high cholesterol need to follow the treatment plan prescribed by their healthcare providers.
Angioplasty and stenting may have to be repeated if the same artery becomes blocked again, a condition called restenosis. If a stent is placed at the time of the angioplasty, the chance of restenosis may be reduced but can still occur.
Only about half of patients with renal hypertension caused by atherosclerosis have their blood pressure successfully treated by angioplasty. By the time the procedure is done, many of these patients have disease in small arteries within the kidney that does not respond to angioplasty.
Angioplasty and vascular stenting for peripheral vascular disease (PVD) affecting arteries in the pelvis and legs are less successful when there are multiple leg vessels that are narrowed or when small vessels have to be opened. Any patient with PVD can benefit from eating a proper diet, getting regular exercise and controlling blood cholesterol.
WHAT CHANGES AM I REQUIRED TO MAKE IN MY LIFE AFTER ANGIOPLASTY?
The chances of restenosis are high and every patient has to undertake preventive measures. Angioplasty or coronary artery bypass surgery; treat the disease only, and not the underlying symptoms.
You are required to incorporate following in your daily routine:
- Familiarize yourself with your family history and after measuring risk profile plan lifestyle changes.
- Eat balanced diet – low in fat.
- Avoid / reduce consumption of alcohol to 30 ml per day only
- Avoid red meat and preferably consume chicken or fish
- Avoid fried foods while preferring baked and fresh food items
- Exercise regularly depending on your age.
- Avoid physical and emotional stress.
- Meditate to control stress.
- Do PRANAYAMA – breathing exercises.
- Undergo regular medical check-ups at specified intervals and ensure controlled lipid profile with low LDL (bad) and high HDL (good) cholesterol.
- If you are a diabetic, ensure controlled blood sugar levels with regular monitoring.
- Regularly take your medication as prescribed by the Doctor.
IN CASE OF RECURRANCE OF SYMPTOMS OF ANGINA – CONSULT YOUR PHYSICIAN IMMEDIATELY. YOUR HEALTH IS IN YOUR HANDS AND YOU CAN AVOID RECURRANCE OF THE DISEASE.